Vaccinations begin in Alabama as COVID-19 cases soar
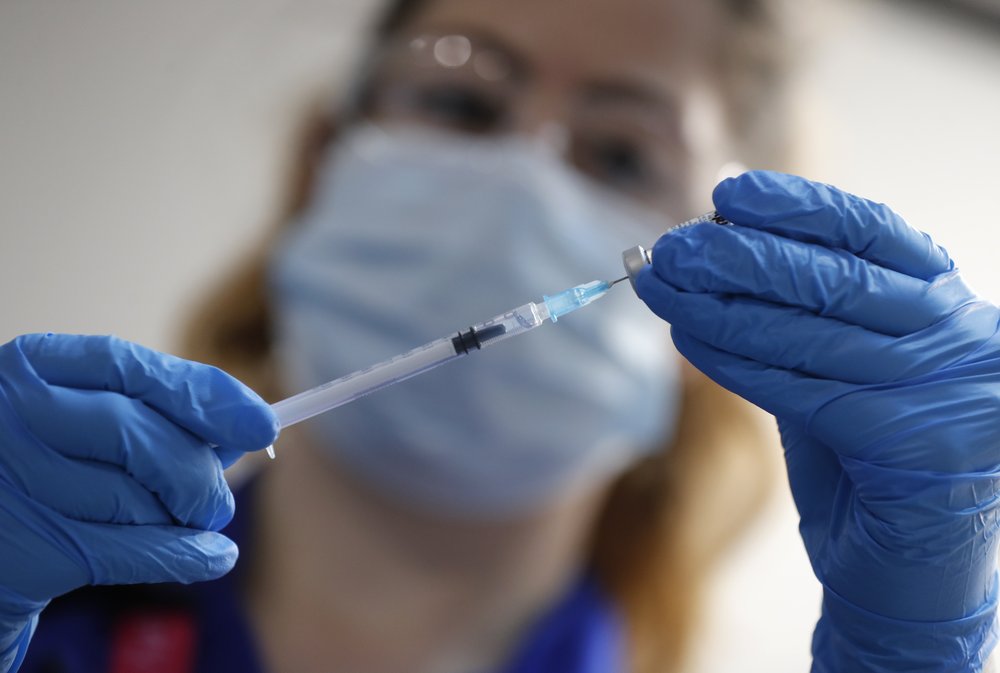
Health care workers began receiving the first vaccinations against the new coronavirus in Alabama on Tuesday as cases of the illness caused by the virus soared. Cullman Regional Medical Center said a longtime nurse, Donna Snow, had received an initial dose of the two-step vaccine a day after the hospital, located north of Birmingham, received its first shipment. “I’m hopeful that more people are able to take the vaccine so we can begin to see a decline in the number of critically ill patients and families impacted by this disease,” Snow, who works in critical care, said in a statement released by the hospital. The Birmingham VA Medical Center said health care workers and veterans at high risk for the disease also would begin receiving vaccinations Tuesday, and additional hospitals will begin providing vaccinations — most to front-line health care workers at first — as more shipments arrive. Workers from the University of Alabama at Birmingham, which is providing vaccinations for multiple organizations across seven counties, will begin giving the first of 11,000 doses on a large scale on Friday, said Dr. Donna Nafziger of UAB Hospital. As many as 1,000 people a day could get the shots. “That’s our goal,” she said. It’s unclear when the vaccine will be available to members of the general public, Nafziger said, but it could be by spring. The state received nearly 41,000 doses of the new Pfizer vaccine in the initial round of shipments. More than 300,000 people in Alabama have contracted the virus, and COVID-19 has killed more than 4,120 people statewide. State health regulators said they have loosened licensing rules to allow more out-of-state doctors to work in the state, where intensive care beds are filling up and medical workers are among the ill. The Alabama Department of Corrections, which has one of the nation’s highest rates of inmate deaths from COVID-19, said three more elderly inmates had died of the illness caused by the coronavirus. All three men had serious health problems before contracting the virus, the agency said in a statement. Republished with the permission of the Associated Press.
Alabama school system issuing $1K COVID-19 bonuses

Full-time employees of an Alabama school system are getting a $1,000 bonus except for its superintendent. The funds will be issued to employees of Baldwin County Schools on Dec, 18, WKRG-TV reported. The money is coming from local funding, primarily sales tax dollars, a spokesman for the school system said. Superintendent Eddie Tyler is not included in the distribution, officials said. In a letter, Tyler said the district has been working on the project for several weeks. The school board approved the recommendation on Tuesday. “I have said over and over how much I appreciate each and every one of you. What you do for this system and the more than 30,000 children we care for, is a monumental task each year. This last year has been well beyond anything anyone could ask of you. While I would like to celebrate the closing of 2020, I fully expect the next year is going to be much of the same,” Tyler said. “This is a drop in the bucket for what you are worth to me.” Republished with the permission of the Associated Press.
Dan Sutter: Who gets vaccinated first?

Vaccines from Moderna and BioNTech/Pfizer are nearing approval by the Food and Drug Administration (FDA). Politicians will now decide who will get vaccinated first. The Centers for Disease Control’s Advisory Committee on Immunization Practices has prioritized vaccination of medical personnel and nursing home residents. The rest of us will have to wait. Prices offer an alternative to political determination of access. However distributed, ramping up vaccine production presents an enormous challenge. The BioNTech and Moderna vaccines both require two doses, so vaccinating all Americans would require over 600 million doses. Production must go from zero to tens of millions of doses per month while maintaining quality. The capacity constraint means that everyone cannot be vaccinated immediately. FDA approval represents a major element of political control. Congress has decided that Americans can only access medicines or vaccines deemed safe and effective by the FDA. Approval moves on bureaucratic time. Britain approved the BioNTech vaccine on December 1; the FDA’s review committee will not meet until December 10. Bureaucrats will not speed up, even with over 1,500 Americans dying daily from COVID-19. Markets would have no legal effectiveness requirement. We could seek out any vaccine or medicine for protection against COVID-19. Liability for unsafe medicines would make drug companies demonstrate safety. Drug companies would cover litigation costs using insurance and no insurer would cover sales without evidence of safety, something resembling the Phase I testing of two vaccines in April and May. With a market, Americans could have gotten vaccinated back in June. Without evidence of effectiveness, initial purchases would likely have been paid out-of-pocket. Vaccinations would have cost “whatever the market will bear;” let’s say $10,000. Drugmakers may have offered the first customers a money-back guarantee: test positive for COVID-19 within six months and get a refund. The first persons vaccinated would then be tracked for evidence of effectiveness. Health insurers and employers (like hospitals) would require evidence, possibly including randomized control trials like those performed this fall, to pay for vaccinations. Insurers would likely require independent collection and examination of the evidence. Once convinced of effectiveness, insurers would pay for vaccinations to save money, to avoid paying for policyholders’ COVID-19 care. Hospitals and nursing homes might vaccinate their employees to assure their customers. Some might decry the wealthy getting vaccinated first, but they would provide a service to the rest of us. The price paid provides drug companies an incentive to ramp up production. They also serve as “volunteers” for testing effectiveness. And once we have evidence of effectiveness, insurers and employers will begin paying. Insurers and hospitals might pay a lot for vaccination – to keep high-risk policyholders healthy or protect high-risk nurses and doctors. High market prices encourage production as quickly as possible without sacrificing quality. A person willing to pay $2,000 in January might only pay $500 for vaccination next July. Vaccine doses delivered sooner will be worth more. The Federal government will purchase at least 100 million doses of each vaccine. These payments will motivate production, yet government projects are often late and over budget. The President and Congress will scream if drug makers fail to deliver on schedule, but will this ensure timely delivery? The United States is not the only country seeking vaccines. Political control means that our politicians could make Americans wait until healthcare workers across the globe are vaccinated. With markets, we must outbid others for vaccination priority. As a wealthy nation, we might seem advantaged in bidding, but rich persons across the globe will pay a lot too. Neither prices nor politics involve magic, so producing the needed doses will take time. Would politics or prices be more effective at producing vaccines as quickly and safely as possible? Politics ultimately involves government bureaucrats procuring vaccines for us. While businesses do not always receive orders on time, bureaucrats will likely keep their jobs even if vaccines are delivered months late. Daniel Sutter is the Charles G. Koch Professor of Economics with the Manuel H. Johnson Center for Political Economy at Troy University and host of Econversations on TrojanVision. The opinions expressed in this column are the author’s and do not necessarily reflect the views of Troy University.
Gov. Kay Ivey extends Safer at Home, mandates masks in public, and warns of ‘dark days’ ahead

Pushback from citizens and political leaders alike has led to controversy over mask-wearing in the state of Alabama. Lieutenant Governor Will Ainsworth, who tested positive for the virus in October, has been resistant to continuing a mask order. He has stated that “masks should be voluntary, not mandatory.” With Covid-19 cases higher than they’ve ever been, Governor Kay Ivey issued her twentieth supplemental emergency proclamation extending the Safer at Home Order that includes a statewide mask requirement. Individuals will be required to wear a mask or other facial covering when in public and in close contact with other people. This order extends until Friday, January 22, 2021, at 5:00 p.m. Except for the extension, all guidelines remain the same. “The mask mandate remains the one stop gap in order to keep the balance of our daily lives and maintaining health and safety,” Ivey stated. “We returned to school, to church, and to work under the conditions of simply wearing a mask.” “These are some of our darkest days since COVID-19 became a part of our daily conversations,” Ivey continued. Ivey posted to Twitter, saying, “Y’all, none of this has been easy. As I have done previously, I cannot thank the people of Alabama enough for the sacrifices you are making-sacrifices for yourself and for others.” Y’all, none of this has been easy. As I have done previously, I cannot thank the people of Alabama enough for the sacrifices you are making—sacrifices for yourself and for others. @ALPublicHealth #alpolitics #TogetherAL 1/7 pic.twitter.com/cbmQ4xK96X — Governor Kay Ivey (@GovernorKayIvey) December 9, 2020 State Health Officer Dr. Scott Harris also spoke at the press conference and discussed the new Covid-19 vaccine rollout. Harris said that infections are “out of control” in much of the country. He said the number of COVID-19 deaths in Alabama is equivalent to a 747 jet crash every month for the past 10 months. “We really are in a difficult time right now in Alabama,” he stated. “This is a very challenging time, and we’re looking at some pretty dark days for the foreseeable future.” Harris said the state expects to receive about 41,000 dozes of Pfizer’s vaccine, possibly within the next week. However, only about 15 hospitals have the capability of storing it. Currently, the Pfizer vaccine has a recommended storage temperature conditions of -70°C±10°C for up to 10 days unopened. This requirement means only certain hospitals can be utilized for storage and distribution. “People have sacrificed so much. It’s been such a difficult year for everybody,” Harris stated. “I would say everybody knows someone who’s been sick from this disease, and most of you know someone who’s died from this disease. We still have some tough weeks ahead of us.”
‘We messed up’: Ex-state senator warns of virus before death

Before his death from COVID-19 former Alabama state senator, Larry Dixon spoke to his wife of 53 years from his hospital bed and asked her to relay a warning. “Sweetheart, we messed up. We just dropped our guard,” Dr. David Thrasher, a pulmonologist and friend of Dixon’s, recalled him saying. Dixon, 78, died Friday from complications of COVID-19. Thrasher said his longtime friend had been mostly careful but may have contracted the virus after gathering with friends. “Larry has been conscientious with masks, doing everything right, social distancing since March… He made one slip up,” Thrasher said. Dixon met with friends at a local restaurant to catch up, and smoke cigars, a social gathering the friends referred to as “prayer meeting.” Three people at the gathering became ill, Thrasher said. “The last thing he told her was, ’Gaynell, I love you. We’ve got to tell people this is real,” Thrasher said. Thrasher said he is telling his friend’s story with the family’s permission in the hopes that people can learn just how easily the virus can spread at casual gatherings. He said it is also important to seek medical care when they first get sick. Alabama and much of the country is seeing a surge in COVID-19 cases following Thanksgiving gatherings. The state in the last two weeks has set records for the number of cases reported each day and the number of people in state hospitals with COVID-19. The state health department has reported more than 276,000 confirmed and probable virus cases and at least 3,942 confirmed and probable virus deaths in Alabama. While the virus causes only mild or moderate symptoms in most people, it can be deadly for the elderly and people with other serious health problems. The hope generated by the imminent arrival of the vaccine is tempered by what medical officials fear will be unchecked spread before it becomes widely available. “I can see the light at the end of the tunnel, but I can also see the locomotive coming at me,” Thrasher said. “The next four months are going to see more devastation and catastrophic problems with public health than we’ve seen probably since 1918. It is going to be very, very bad.” Dixon was the executive director of the Alabama Board of Medical Examiners from 1981 until his retirement in 2016. A Republican, Dixon was elected to the Alabama House of Representatives in 1978 and the Alabama Senate in 1983. He retired from the Alabama Legislature in 2010. Republished with the permission of the Associated Press.
Dan Sutter: Are we paying twice for COVID medicines?

Two vaccines appear highly effective against SARS-CoV-2, and remdesivir is helping doctors treat severe COVID cases. These products raise challenging questions regarding patents and government funding of research. If taxpayers fund a medical breakthrough, should we then have to pay for the medicine? Consider Gilead Science’s remdesivir, which effectively treated COVID in a clinical trial. The National Institutes of Health (NIH) and the Defense Department funded the drug’s development. Public Citizen estimates that public funding totals at least $70 million. They argue that remdesivir should be priced at cost because taxpayers “should not have to pay twice” for it. Before addressing this question, let’s consider the rationale for patents. Patents help ensure the funding of research producing knowledge. Medicines and vaccines are ultimately knowledge that a given combination of chemicals keeps us from getting sick or restores our health. Research must be performed to generate new knowledge and is highly uncertain; experiments do not always yield breakthroughs. The prices of successful medicines and vaccines must cover the cost of all this research. Knowledge is challenging to market. Imagine trying to sell some new fact which nobody else knows. The first person buying this new fact can then sell it to others, undercutting the price you need to charge to recover your research costs. For a medicine, a chemist can analyze a sample to determine the formula, while scientists can reverse-engineer new products. Patents provide inventors exclusive rights to their inventions for a limited number of years. The patent prohibits copying of the invention. Ideally, the patent should be only long enough to encourage research, but calculations cannot be made with precision. Both businesses and the Federal government fund research. The NIH spends $40 billion a year on medical research. Successful medical researchers typically must win NIH grants. The public-private division of research is in principle along the line between basic and applied research. Business funding typically becomes available when knowledge is close to yielding a marketable product; this is applied research, or the development part of R&D. Basic research advances knowledge for knowledge’s sake. Although as fundamental breakthroughs percolate through society, people begin to recognize the practical applications, the commercial value of basic research is frequently too remote to attract investors. We can see how taxpayers could “pay twice” for new medicines. If a new medicine were developed almost entirely through government funding, the company marketing the drug needs profits to recover its negligible research expenses. Most medicines though – and new products generally – require a mix of research and development. Even if the Federal government funds the basic research, a lot of work remains to yield a commercially valuable product. The Moderna and BioNTech SARS-CoV-2 vaccines illustrate this. Both use messenger RNA vaccines, and the NIH funded the basic research on m-RNA. The breakthrough has offered enormous promise for 25 years but prior to 2020 no medicines on the market. Turning m-RNA into medicine involved further breakthroughs to encase bioengineered proteins in lipid nanoparticles. Moderna and BioNTech have done much of this last portion of the research. What about the estimated $10 billion in Federal spending on COVID vaccines through Operation Warp Speed? This has covered the testing and production of vaccines. Manufacturing is distinct from the knowledge contained in a candidate vaccine, and patents reward knowledge creation. Knowledge drives our prosperity. More important than the mix of public versus private sector research is the discovery of new knowledge. COVID-19 has revealed a very healthy global biomedical research industry. Remdesivir and other treatments have reduced the fatality rate among hospitalized patients by an estimated 70 percent since March. And researchers formulated two seemingly highly effective vaccines within weeks of the identification of the novel virus’ DNA. Taxpayers should not have to pay twice for the same medicine. Yet politicians have protected health at enormous cost during the pandemic. Overpaying for effective vaccines or medicines is frustrating but preferable to going without. Daniel Sutter is the Charles G. Koch Professor of Economics with the Manuel H. Johnson Center for Political Economy at Troy University and host of Econversations on TrojanVision. The opinions expressed in this column are the author’s and do not necessarily reflect the views of Troy University.
Alabama Rep. Robert Aderholt in quarantine over COVID-19

Republican Rep. Robert Aderholt said he is in quarantine and will miss votes this week after being potentially exposed to COVID-19. Aderholt, who won a 13th term representing much of north Alabama earlier this month, said in a statement released by his office Sunday that we was in close contact for several hours with someone who subsequently tested positive for the illness caused by the new coronavirus. Based on advice from the House physician, Aderholt said he would quarantine in Alabama and get another test later this week rather than return to Washington, D.C. “Unfortunately, this also means I will have to miss votes this week, but the safety of my staff and colleagues is far more important, and I could possibly still expose someone,” said Aderholt, of Haleyville. Aderholt, 55, said he did not have any symptoms of COVID-19. Republished with the permission of the Associated Press.
50 Department of Education employees quarantined after COVID-19 outbreak
Alabama State Superintendent of Education Eric Mackey announced Thursday that 50 Department of Education employees had been placed on quarantine after a coronavirus outbreak in the DOE building. According to AL.com, most employees are from one section of the building, so the entire section was quarantined and will be working from home. One worker from another section tested positive, so that group was sent home as well. Most employees who tested positive didn’t have any symptoms. The first section of employees will be coming back into the office in the next few days. After they return, there will be fewer than 10 employees left in quarantine. However, this outbreak is definitely indicative of a spike in cases, even with steps in place to prevent the spread of the virus. Employees have been asked to stay in their sections and not walk around too much in other areas of the building to prevent the virus’s spread. “To put it in perspective, between March 13 and 11 days ago, we had 12 total cases of the virus among employees here,” Mackey commented. “So we did pretty good for seven months. And in those 11 days, we’ve had nine or ten more cases.” During the summer, the number of employees in the building was cut in half. This option is being discussed again as a way to prevent another outbreak. Mackey did note that while most state education departments haven’t returned to buildings since March, Alabama hasn’t had a problem until November. “It can happen so fast, when you go from one to two to four to eight in a day,” Mackey said. “And that’s what happened to us a couple weeks ago.” Meanwhile, other counties are responding to outbreaks as well. Sparkman Middle School and Harvest Elementary will go to online learning. All other schools will remain open. Superintendent Allen Perkins announced Thursday that students from those schools would move to virtual learning starting Monday, November 16, with students returning to school on November 30. 68 coronavirus deaths were reported on Wednesday; however, it was announced on the BamaTracker Twitter page that the deaths didn’t all happen in a single day. “Please remember that while ADPH reported 68 deaths yesterday, they were spread out over the months prior. Many many media outlets are running with the story they all occurred yesterday. Even ADPH acknowledged this was not the case.” Please remember that while ADPH reported 68 deaths yesterday, they were spread out over the months prior. Many many media outlets are running with the story they all occurred yesterday. Even ADPH acknowledged this was not the case. — Bama Tracker: Alabama COVID-19 (@BamaTracker) November 12, 2020
Martha Roby: COVID-19 will not shake our democracy

Election Day is here, and it’s safe to say that this year’s election looks quite different than those of the past. As we continue to navigate the ongoing Coronavirus (COVID-19) pandemic, several protocols have been put in place nationwide to create cautious and healthy environments for in-person voting. A record-breaking number of Americans have already voted or plan to vote in the 2020 General Election, with over 75 million individuals having cast their ballots. An estimated 4.9 million people live in the state of Alabama. In the 2020 March Primary Election, there was a total of 3,576,107 Alabamians registered to vote. Of those registered to vote, approximately 1,176,315 individuals – or 33 percent – actually exercised their right to vote in this year’s primary. On Thursday, the Alabama Secretary of State’s office announced that more than 259,200 Alabamians had voted by absentee, and Secretary of State John Merrill stated that 316,130 ballots had been requested. While the final statewide voter turnout will not be known until after Tuesday’s election, it is vital we each take the time to exercise our right to vote as afforded to us by the U.S. Constitution. If you plan to vote in-person, please be sure to follow all local and statewide COVID-19 guidelines. Your participation is especially crucial as the number of daily new Coronavirus cases across the state are on the rise. For COVID-19 voting resources and information, visit sos.alabama.gov/covid-19-voting-resources. The United States was founded on a strong set of principles that have shaped our nation and guided the American people for nearly 250 years. We will not allow a health pandemic to shake our democracy. We have been given the right to freely and openly express our beliefs and opinions, participate in civil public discourse, and vote to elect the individuals who lead our nation. If you have not already, I encourage you to exercise your right to vote and participate in the democratic process. Martha Roby represents Alabama’s Second Congressional District. She lives in Montgomery, Alabama, with her husband Riley and their two children.
After improvement, virus cases worsening in Alabama

The coronavirus pandemic appears to be worsening again in Alabama after weeks of improvement as residents grow weary of preventive measures that slowed the spread of the disease after a summertime peak, health officials said. Donald Williamson, the president of the Alabama Hospital Association, said he has noticed fewer people wearing masks and trying to stay away from each other in public over the last couple weeks, and such changes seem to be showing up in troublesome statistics. “I think it’s clear that we all have COVID fatigue,” Williamson said in an interview Tuesday. Dr. Ellen Eaton, a disease expert at the University of Alabama at Birmingham, tweeted that average daily hospitalizations, deaths, the transmission rate of the virus and positive tests all were rising “just as flu season arrives.” More than 2,800 people have died from COVID-19 in the state, which ranks 20th highest in the nation for fatalities on a per-person basis, and about 174,000 have tested positive, according to researchers at Johns Hopkins University. The virus has been spreading at a quickened pace since early October, figures show, and around 840 people have been hospitalized a day over the past week, compared to around 750 a day in late September. The state’s situation is much better than in the summer, when hospital intensive care beds were nearly full and the virus was spreading out of control, Williamson said. The state’s virus caseload fell and stabilized after Gov. Kay Ivey and health officials imposed a statewide mask order that will extend at least into November. It could take about four weeks to determine whether Alabama is headed toward a new, elevated plateau or another uncontrolled spike that could fill up hospital beds once again, Williamson said, but neither are good as flu season gets closer and cases of COVID-19 are on the rise in a majority of states. “Things are not going well,” he said. While the virus causes only mild or moderate symptoms for most people, it can be deadly for the elderly and people with other health problems. Republished with the permission of the Associated Press.
Inmate dies after contacting COVID-19

A 74-year-old inmate at an Alabama prison has died after contracting COVID-19, the 26th inmate to die after contracting the virus. The Alabama Department of Corrections said in a news release that Johnny Dwight Terry, a 74-year-old inmate at Limestone Correctional Facility, died Thursday. The prison system said Terry was transferred to a hospital on Tuesday after showing symptoms of the disease. He died two days later. Terry had multiple preexisting medical conditions, according to the prison system. Terry was serving a life sentence on a murder conviction from Lawrence County, the agency said. The state prison system has reported coronavirus cases in 21 out of 26 facilities. Alabama has documented 441 cases of coronavirus among the state prison population to date, according to the prison system. The Department of Corrections said 33 cases are currently active. There have been 415 cases among prison employees and 44 remain active. Two employees have died, according to the prison system. Republished with the permission of the Associated Press.
White House official praises Alabama virus response, tells men to wear masks

Dr. Deborah Birx noted a gender gap as she traveled the state in mask wearing, one of the tools to curb the spread of the virus.

