New U.S. hospitals face fiscal crisis over COVID relief money

A whole town celebrated in 2020 when, early in the coronavirus pandemic, Thomasville Regional Medical Center opened, offering state-of-the-art medicine that was previously unavailable in a poor, isolated part of Alabama. The timing for the ribbon-cutting seemed perfect: New treatment options would be available in an underserved area just as a global health crisis was unfolding. In the end, that same timing may be the reason for the hospital’s undoing. Now deep in the red two years into the pandemic, the 29-bed, $40 million hospital with a soaring, sun-drenched lobby and 110 employees is among three medical centers in the United States that say they are missing out on millions in federal pandemic relief money because the facilities are so new they lack full financial statements from before the crisis to prove how much it cost them. In Thomasville, located in timber country about 95 miles (153 kilometers) north of the Gulf Coast port of Mobile, hospital officials have worked more than a year to convince federal officials they should have gotten $8.2 million through the CARES Act, not just the $1 million they received. With a total debt of $35 million, the quest gets more urgent each day, said Curtis James, the chief executive officer. “No hospital can sustain itself without getting the CARES Act money that everybody else got,” James said. Employees are trying to save money by cutting back on supplies but residents including Judy Hutto are worried about the hospital’s future. Hutto drove there recently for tests from her home 15 miles (24 kilometers) out in the country. “The areas need it,” she said. “It’s a nice hospital.” CEO Barry Beus also is trying to plug a gap at Rock Regional Hospital, located south of Wichita in Derby, Kansas. The hospital is due as much as $15.8 million, officials said, but because it only opened in April 2019 and lacks complete pre-pandemic financial statements, it has received just a little more than $985,000. The only thing that’s saved the facility from financial ruin so far is the cooperation of doctors, contractors, and vendors who haven’t pushed for payments, he said. “If we lose them, we lose the hospital,” said Beus. Three Crosses Regional Hospital opened in 2020 in Las Cruces, New Mexico, and piled up a staggering $16.8 million in losses in just three quarters while receiving only $28,000 in aid, said Landon Fulmer, a Washington lobbyist working with all three hospitals to obtain additional funding. Each facility is being penalized for being new even though they provided the same costly COVID-19 care as other medical centers and lost revenue from other procedures including elective surgeries, he said. “It really is quite a strange situation in a way, one that shouldn’t have happened,” Fulmer said. With about 420,000 health care providers nationwide already receiving assistance from a $178 billion pot, the government isn’t covering 100% of losses for anyone, said Chris Lundquist, a spokesman for the U.S. Health Resources and Services Administration, which is overseeing the program. “HRSA has strived to provide as much support as possible to as many hospitals as possible within the limits of the law and funding,” he said. The agency said it used proxy financial information for hospitals that opened in 2019 or 2020 to create an equitable payment system. “They have all received funding,” said Lundquist. While virtually all the aid money is spoken for, Lundquist said hospitals seeking additional aid can go through an appeals process. Hospitals also can seek a supplemental appropriation or funding in the upcoming fiscal years, he said. All three of the hospitals say they deserve more. Officials in Thomasville are trying to leverage congressional influence. Mayor Sheldon Day has made several trips to Washington, D.C., to speak with members of the state’s congressional delegation and health officials, and the president of the Alabama Hospital Association, Dr. Don Williamson, has contacted the White House seeking help. “They’ve been assured they’re going to be taken care of. But the fact is, when you’re dealing with government entities, you don’t have the money until you have the money,” said Williamson. Located in southwest Alabama, Thomasville lies within an impoverished area called the Black Belt. About 70% of Black Belt residents qualify for Medicare or Medicaid, and health care has been limited for generations. The last hospital shut down in Thomasville more than a decade ago, leaving only hospitals that offer fewer services in the surrounding region. Officials worked for years to secure a new hospital so residents wouldn’t have to drive 90 minutes for high-tech services such as digital imaging, full surgical options, echocardiograms, 3D mammography, and more. Using a partnership between the city and a municipal health care authority, Thomasville Regional secured federal funding from the Department of Agriculture and opened on March 3, 2020, before cases of COVID-19 caught fire in the rural South. “We thought we were off to a good start,” said James, the chief executive. “And then everything shut down.” Patients stopped showing up for scans, elective surgeries, mammographies, and other moneymaking services because of pandemic shutdowns, and financial reports that looked promising turned perilous within weeks. Recognizing that new hospitals couldn’t calculate COVID-19 losses because they couldn’t compare 2020 numbers with past years, Health and Human Services allowed hospitals to use budget numbers for calculations rather than prior financial statements. That’s how the hospital determined that it was missing out on more than $7 million in aid, James said. While the hospital is still waiting on that aid, he said, the government did agree to provide $1 million in assistance that went to all other hospitals. “That was OK, but other hospitals that are in our region got $8 million, $9 million,” he said. The Birmingham-based Medical Properties Trust recently gave the hospital $2 million and James said leaders are confident Thomasville Regional will eventually get the extra federal aid. “But it will take time,” he said. Like Thomasville Regional, Rock Regional in Kansas saw revenues dry up soon after
Kay Ivey awards $80 million in COVID-19 relief funds to hospitals and nursing homes

On Wednesday, Gov. Kay Ivey awarded an additional $80 million of the State Fiscal Recovery Fund from the American Rescue Plan Act (ARPA) to provide reimbursements for the state’s hospitals and nursing homes. These funds will support two grant programs of up to $40 million each, one administered by the Alabama Hospital Association and the other by the Alabama Nursing Home Association. Alabama received $2.1 million in ARPA funds, and the Alabama Legislature appropriated $80 million from Alabama’s State Fiscal Recovery Fund for these programs. “Alabama is showing the rest of the country that we can learn to live with this virus and move on with living our lives. As we close the door on this thing, I once again give my utmost appreciation and thanks to the medical professionals and staff in our hospitals and nursing homes across the state,” stated Ivey. “These men and women, no doubt, deserve our praise for getting us through this. I commend the Alabama Legislature for appropriating these dollars to continue helping our hospitals and nursing homes get back on their feet.” Don Williamson, MD, President and CEO of the Alabama Hospital Association applauded Ivey’s efforts to provide funding to Alabama’s hospitals. “For two years, Alabama’s hospitals and their staff have remained at the forefront of pandemic response, providing care to their communities 24-hours-a-day, 7 days a week” stated Williamson. “Alabama’s hospitals are grateful for the $40 million appropriated during the most recent special session. This financial assistance is part of the ongoing commitment of the administration and the Alabama legislature to ensure Alabama’s hospitals remain operational, preserving access to care for all Alabamians.” Brandon Farmer, Alabama Nursing Home Association President & CEO, thanked Ivey for her efforts to help patients and residents receive high-quality care. “On behalf of Alabama long-term care sector, I thank Governor Ivey, the Alabama Legislature and the Department of Finance for allocating these funds to nursing homes and their consistent support throughout the pandemic,” stated Farmer. “Governor Ivey has shown unwavering support to nursing homes throughout the pandemic. These funds will enable nursing homes to continue their recovery and provide the high-quality care patients and residents deserve.”
COVID-19 hospitalizations decline 5% across Alabama
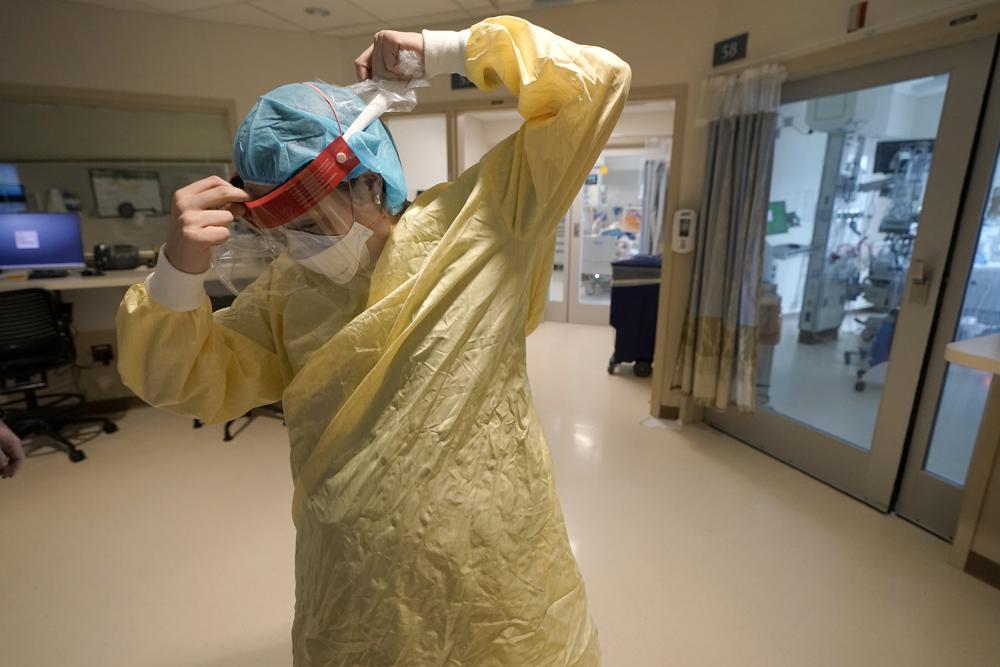
The number of people hospitalized with COVID-19 has decreased about 5% in Alabama since last week, a potential sign of improvement in the fight against the pandemic. Statistics from the Alabama Department of Public Health showed 2,805 people were being treated for the illness on Monday, down from 2,961 last Tuesday. Hospitalizations increase or decrease daily, and some hospitals are still struggling with an influx of illness, patients in intensive care on ventilators, and staff shortages. But the percentage of people testing positive for COVID-19 dropped to a still-high 36% after exceeding 40% for nearly four weeks straight. “Things are not getting worse,” said Don Williamson, president of the Alabama Hospital Association. The entire state remains in the danger zone with high levels of community transmission, yet the improvement has some health officials hopeful amid a wave of illness linked to the highly-contagious omicron variant and Alabama’s low vaccination rate. About 49% of the state’s population is fully vaccinated, and 33% have had booster doses, according to federal statistics. Moore than 17,000 people have died from COVID-19 in the state, giving Alabama that nation’s fourth-highest death rate from the illness. Over the past two weeks, the rolling average number of daily new cases has increased by 14,114.5, or about 127%. Republished with the permission of the Associated Press.
Harris: ‘Omicron spreading like wildfire’ in Alabama

Alabama’s state health officer on Tuesday said the highly infectious omicron variant of COVID-19 is spreading like wildfire in Alabama as the state sets record numbers for cases. “We are unfortunately not in a real good place right now. We are seeing the highest daily case numbers we have seen since the pandemic began,” State Health Officer Scott Harris said in a briefing with reporters. “It is just spreading like wildfire,” Harris said, adding that, “omicron will infect a very large number of people in Alabama before it finally subsides.” Alabama set new records for daily cases, hitting more than 8,000 a day December 30 and December 31, according to numbers from the Alabama Department of Public Health, and the average percentage of COVID-19 tests coming back as positive hit a new high of 38.5% Tuesday. “So, we really need people to do the single most important thing they can do which is to be fully vaccinated and boosted when it’s appropriate to do so.” While early research suggests omicron causes less severe disease than earlier variants — such as the delta variant which he said had an estimated 2% fatality rate — he cautioned that some people will still get severely ill and the high infection rates means significant numbers could end up in state hospitals. “We had 41 people die yesterday. We don’t have that with the flu. We don’t have that with common colds. It’s just not the same thing,” Harris said. According to researchers at Johns Hopkins University, the seven-day rolling average of daily new cases in Alabama has risen over the past two weeks from 831.71 new cases a day on December 19 to 6,139.43 new cases a day on Sunday. The state ranks 29th in the country for new cases per capita. There were more than 1,100 people in state hospitals with COVID-19 on Monday, although that is far fewer than the 3,000 people hospitalized at the peak of earlier waves. Dr. Don Williamson, president of the Alabama Hospital Association, on Monday said about 32% of hospitalized patients had been vaccinated, but he did not yet have numbers on what percentage had booster shots. Williamson said the number of medical workers who are out because of COVID-19 or flu is “creating some staffing issues” at hospitals across the state. Less than 48% of the state’s population is fully vaccinated, giving Alabama one of the nation’s lowest vaccination rates despite months of work by health officials to promote the shots. With more than 16,450 dead of the illness, Alabama has the nation’s third-highest death rate from COVID-19, according to researchers at Johns Hopkins University. Many Alabama students returned to K-12 classrooms this week, although some systems opted for temporary remote learning. The Alabama Department of Public Health recommends students and educators wear masks, guidance that has remained unchanged. The University of Alabama announced this week that people will be required to wear masks in most campus settings. Republished with the permission of the Associated Press.
Some schools teaching online, requiring masks as cases surge

With Alabama hospitals treating more COVID-19 patients daily and the positivity rate for coronavirus tests exceeding 35% statewide, some state school systems are returning to online learning or implementing mask restrictions to avoid classroom outbreaks. In Sylacauga, students will attend classes remotely for three days when the new semester begins on Wednesday, Superintendent Michele Eller said in a statement. “Considering the surge right here in our community following the holiday gatherings, this is the reasonable course of action to protect our students and teachers from exposure,” she said. Shelby County schools in metro Birmingham started the post-holiday grading period online Monday for its nearly 21,000 students as part of a plan implemented before the latest surge. The system did the same thing last year to allow for additional quarantine time for anyone who might have been exposed to the virus or gotten sick over the break. Pike County’s public schools will hold classes in person but require masks for all workers and students through January 28, officials said in an announcement on social media. “Our focus will remain on keeping our students and employees safe. By implementing these steps, we hope to keep our schools open through this surge,” said the system located in southeast Alabama. More than 1,100 people were hospitalized statewide with COVID-19 on Monday, or more than 3.5 times as many as in mid-December. About 36% of COVID-19 tests came back positive statewide over the last week — a high for the pandemic — and the positivity rate exceeds 40% in 10 of the state’s 67 counties, according to statistics from the Alabama Department of Public Health. “Community transmission is just spreading like wildfire right now,” said Dr. Sarah Nafziger, vice president of clinical support services with UAB Health System. Less than 48% of the state’s population is fully vaccinated, giving Alabama one of the nation’s lowest vaccination rates despite months of work by health officials to promote the shots. With more than 16,450 dead of the illness, Alabama has the nation’s third-highest death rate from COVID-19, according to researchers at Johns Hopkins University. The rolling average number of daily new cases has increased by about 5,004 over the past two weeks, a jump of about 630%. There were nearly 1,058 new cases per 100,000 people in Alabama over the past two weeks, which ranks 20th in the country for new cases per capita. Hospitalizations aren’t increasing as quickly as the overall COVID-19 case total, apparently because the highly contagious omicron variant doesn’t make patients as sick as earlier versions of the virus, Nafziger said. But the latest surge is still straining health systems because of the large number of workers who are being exposed to the highly contagious variant or infected, she said. “We’re having a lot of staff who are testing positive, who are having to stay out of work because of that,” said Nafziger. Dr. Don Williamson, president of the Alabama Hospital Association, said the number of medical workers who are out because of COVID-19 or flu is “creating some staffing issues” at hospitals across the state. “It’s just a much more transmissible virus,” Williamson said of the omicron variant. “I worry that as our cases continue to rise, we are going to see more and more people in the hospital, and it’s going to happen when staffing was already challenging.” Williamson said that even though omicron seems to be less severe, it is wrong to dismiss the variant as the equivalent of a cold. There are 210 COVID-19 patients in hospitals, about double the amount at the beginning of the month. “If you believe that this variant is nothing more than the common cold, you are mistaken because we don’t hospitalize for the common cold. Yet, we are seeing patients with this surge being hospitalized at increasing rates,” Williamson said. “Based on what we’re seeing, there are fewer people who get severe disease, but there are clearly some who get severe disease.” Republished with the permission of the Associated Press.
Alabama hospitals face severe blood shortage, need donations
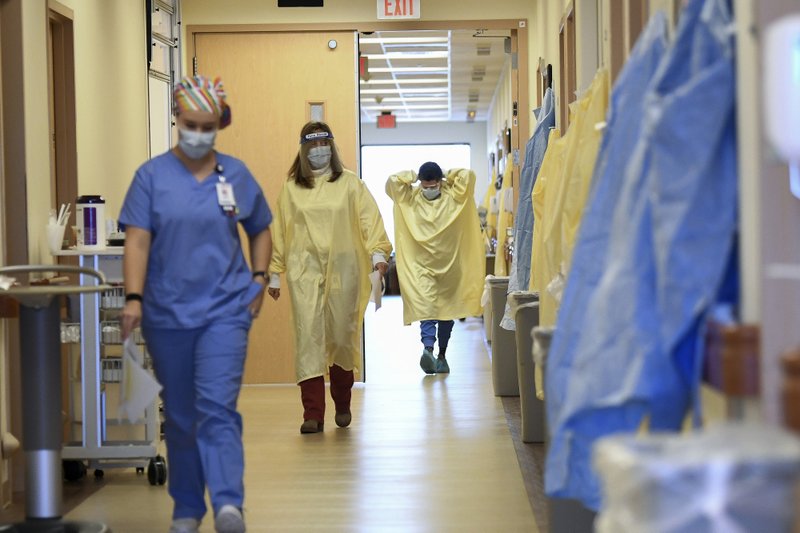
Alabama hospitals are facing a severe blood shortage and have a critical need for donations, an organization of state hospitals said. The Alabama Hospital Association said the state is facing a blood supply crisis after the number of people donating blood has declined during the COVID-19 pandemic. “The shortage of blood has reached a crisis level. We have critical shortages now throughout the health system,” said Dr. Don Williamson, the president of the Alabama Hospital Association. The Hospital Association said LifeSouth, the donation center that supplies blood to the majority of Alabama’s hospitals, has listed the statewide blood supply at “critical” levels. That means, on average, there is less than two days’ supply of blood on their shelves. Williamson said some hospitals would have difficulty handling a major trauma event as a result. That is particularly concerning with the holiday travel season approaching, he said. While it’s not uncommon to see occasional blood shortages on a local level, Williamson said, “It’s pretty rare for us to see this level of blood shortage on a statewide basis.” The hospital organization said donations are urgently needed. The group also encouraged schools, colleges, churches, businesses, and other organizations to host a local blood drive as soon as possible. “We are strongly encouraging people who can donate, to please go donate,” Williamson said. Republished with the permission of the Associated Press.
Record for virus patients in Alabama intensive care units

Alabama has set a new high for the number of COVID-19 patients in intensive care, although the total number of hospitalized coronavirus patients remains slightly below the winter peak. The state on Sunday had 884 COVID-19 patients in intensive care, according to the Alabama Hospital Association, the highest number since the pandemic began. Dr. Don Williamson, the former state health officer who heads the organization, said the previous high was 848 in January, according to his numbers. “I clearly think that is a record,” Williamson said of the latest figure. The total number of the virus patients in state hospitals was 2,829 on Monday, still below the pandemic high-water mark of 3,087 set in January. “I’d love to think that we are not going to get to the 3,000 that we saw in January, but I don’t have a scientific reason to think we won’t,” Williamson said. The number of virus patients requiring intensive care is a worrying sign, but the state is seeing some improvements in other areas, including vaccination rates. While Alabama has one of the lowest vaccination rates in the country, the state moved out of last place to slightly ahead of Mississippi for the percentage of the population that is fully vaccinated. According to the Centers for Disease Control and Prevention, about 38.1% of Alabamians are fully vaccinated. With older populations more likely to be vaccinated, state hospitals say they are seeing more younger patients with COVID-19 as the contagious delta variant sweeps across unvaccinated groups. East Alabama Medical Center posted on social media about the age breakdown of ICU patients. Of the 25 COVID-19 patients in ICU at the hospital, 14 are under age 60. Of those 14, seven are in their fifties, four are in their forties and three are between the ages of 20 and 39. The hospital has 20 patients on ventilators, of which all but three are unvaccinated. Republished with the permission of the Associated Press.
Nearly 200 inmates test positive for COVID at Alabama prison

Nearly 200 inmates tested positive for COVID-19 at a state prison after officials implemented mass testing in the wake of an outbreak at the facility. The Alabama Department of Corrections said in a news release that all Elmore Correctional Facility inmates not currently exhibiting symptoms were tested last week. Out of the 960 asymptomatic inmates, 191 tested positive for COVID-19. Elmore is a medium-security prison that houses about 1,000 inmates. The prison system said the testing was done as a precautionary measure in response to a recent increase in cases at the prison. Since the pandemic began, 1,901 total cases of COVID-19 have been confirmed among inmates, and 224 of those remain active. Sixty-six inmates and three staff members have died, according to numbers provided by the prison system. The Alabama prison system suspended visitation during the pandemic and has not said when it will return. Alabama has seen a surge in COVID-19 cases fueled by the highly contagious delta variant and the state’s low vaccination rate. Case and hospitalization numbers are quickly approaching what they were at the winter peak of the pandemic. The number of hospitalized patients with COVID-19 was 2,723 on Tuesday, a figure that is nearing the previous peak of 3,087 patients on Jan. 12. There are now more patients needing intensive care than there are intensive care beds in the state. The state on Tuesday had 11 more patients in intensive care than the state had intensive care beds, according to Dr. Don Williamson, the former state health officer who now heads the Alabama Hospital Association. Many hospitals have implemented surge plans and are housing intensive care patients in other areas of the hospital. Republished with the permission of the Associated Press.
Kay Ivey issues state of emergency as hospitals face COVID surge

Alabama Gov. Kay Ivey on Friday issued a state of emergency as state hospitals face a surge in COVID-19 cases, an order that came the same day the state tied a record low for available intensive care unit beds. Ivey issued a limited state of emergency aimed at giving medical providers flexibility on staffing and capacity decisions and easier shipment of emergency equipment and supplies. The Republican governor stressed she would not be issuing any closure orders or mask mandates. ”I want to be abundantly clear: there will be absolutely no statewide mandates, closures, or the like. This state of emergency is strategically targeted at removing bureaucracy and cutting red tape wherever we can to allow our doctors, nurses, and hospital staff to treat patients that come through their doors,” Ivey said in a statement. The order came as medical providers described a “tidal wave” of COVID-19 cases that is putting severe stress on Alabama hospitals. The state on Friday tied the record low for available intensive care unit beds with just 39 vacant beds statewide, said Dr. Don Williamson, the former state health officer who now heads the Alabama Hospital Association. “The system is slowly becoming overwhelmed,” Williamson said. Of the state’s 1,567 intensive care unit beds, 689 are filled with COVID-19 patients, and just 39 are empty. Alabama ranks fifth in the country for new cases per capita, according to researchers at Johns Hopkins University. The state on Friday also saw a record number of pediatric cases with 40 children hospitalized with COVID-19, Williamson said. Williamson said the emergency declaration will allow hospitals to take steps such as expanding facilities or opening an antibody infusion center without getting state permission. It will increase the number of nurse practitioners and other staff positions that a doctor can supervise. Medical officials have said a surge in cases is being driven by low vaccination rates and the highly contagious delta variant and implored people to get vaccinated and wear masks to combat the spread and prevent severe illness. Alabama has one of the lowest vaccination rates in the country. “Unlike last year when we were hoping for a miracle, our greatest weapon against COVID-19 today is the vaccine, so, if you can, roll up your sleeve and get the shot,” Ivey said. Dr. Sarah Nafziger, vice president of the University of Alabama at Birmingham Hospital Clinical Services, said Thursday that the hospital has had to limit the number of procedures they are doing and decline transfers to the hospital. “We are seeing an absolute tidal wave,” Nafziger said. She said the hospital is providing care and emergency services, but she said the trends and projections are alarming. “When you think about running out of hospital beds and running out of health care resources, that is the path that we are on.” Republished with the permission of the Associated Press.
Alabama’s COVID hospitalization levels highest since January
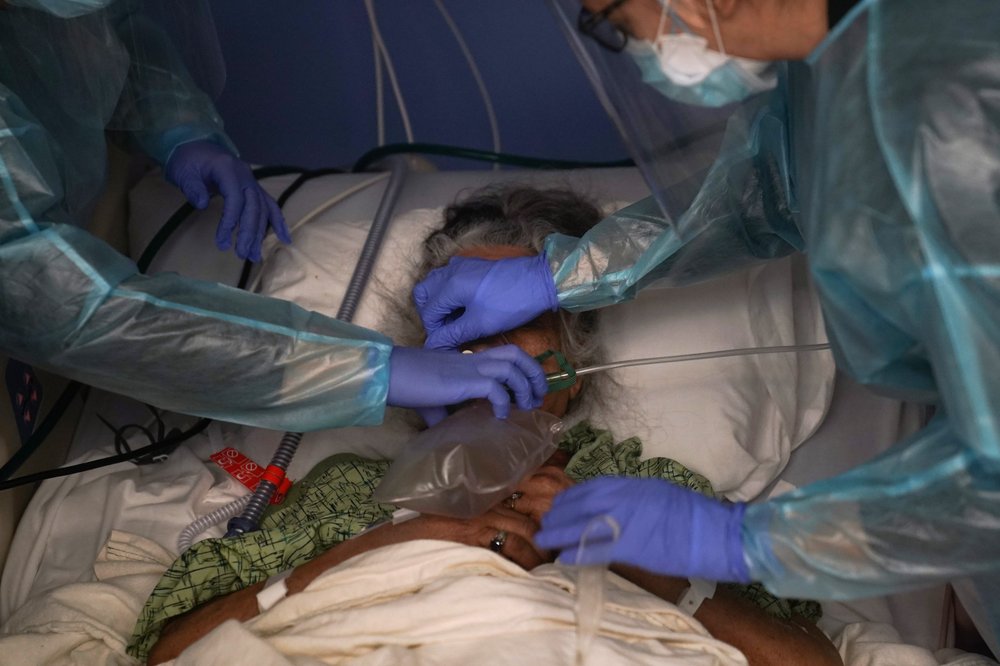
Alabama is racing toward virus numbers it last saw at the peak of the pandemic, with more than 2,100 COVID-19 patients in state hospitals Monday and only 6% of intensive care unit beds available, a medical official said. Medical officials have said low vaccination rates and the highly contagious delta variant have combined to cause an explosion of cases. “It’s like the California wildfires. We have the perfect environment,” said Dr. Don Williamson, Alabama’s former state health officer who now heads the Alabama Hospital Association. On Monday, there were 2,134 patients with COVID-19 in state hospitals, including 33 children, according to numbers provided by the Alabama Hospital Association. Nearly one-third of the hospitalized virus patients, or 628, are in intensive care units and 318 patients are on ventilators. Williamson said 42% of intensive care unit beds in the state are now occupied by someone with COVID-19. The current hospitalization number of 2,134 is lower than the little more than 3,000 recorded at the peak of the pandemic in January. However, health officials have expressed concern about the steep upward trend. A month ago, there were 247 virus patients in state hospitals, according to numbers compiled from the Alabama Department of Public Health. “It’s filling up faster and there is no end in sight,” Williamson said. The state had 87 intensive care unit beds available Monday, or 6%, Williamson said. By comparison, the state had 3% available at the worst part of the pandemic in January. One hospital administrator described patients begging to be vaccinated, only to be told that it is too late. Already full with patients being treated for usual medical ailments like heart attacks, strokes, or trauma injuries, Decatur Morgan Hospital also is treating 26 COVID-19 patients, up from 15 last week, president Kelli Powers said during a news conference Monday. The ill included a 38-year-old person who is on a ventilator in intensive care, she said, and the sickest patients infected by the virus are not vaccinated. “We have a lot of people who are on their deathbeds begging for the vaccine, but at that point, it’s too late,” she said. Health care workers are exhausted after months of combatting the illness, she said, and the best way to stem the surge is for more people to get shots. It’s one thing to care for a patient who got a vaccine and still got COVID-19, she said. “But for someone to just not take the vaccine and then get really, really sick, I think that’s frustrating. But it’s also depressing at some point to know that someone might not live,” Powers said. According to researchers at Johns Hopkins University, the seven-day rolling average of daily new cases in Alabama has nearly doubled over the past two weeks from 1,495 new cases a day on July 24 to 2,829.14 new cases a day on Saturday. Alabama ranks fifth in the country for new cases per capita, behind Florida, Louisiana, Arkansas, and Mississippi. Republished with the permission of the Associated Press.
Birmingham hospitals: Most COVID patients are unvaccinated
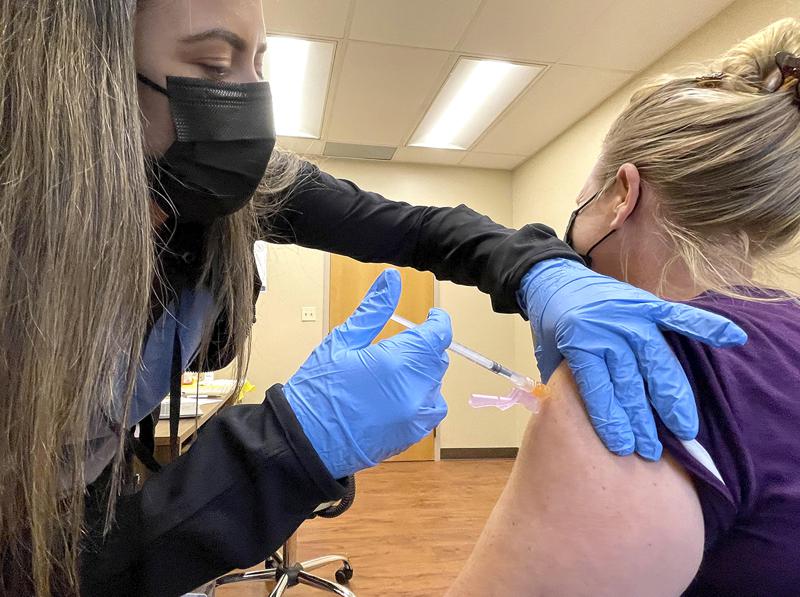
Hospitals in Birmingham are seeing a surge in COVID-19 patients — usually unvaccinated and often younger — as doctors and administrators pleaded Wednesday for people to get vaccinated. Doctors and administrators at seven Birmingham hospitals participated in a media briefing to discuss the recent surge in cases. The overwhelming majority of current COVID-19 patients are unvaccinated, and patients tend to be younger than they were at the start of the pandemic before vaccines were available, the hospital’s officials said. Dr. Elizabeth Ennis, chief medical officer of Brookwood Baptist Health, said the delta variant of the virus is moving like “wildfire” through the state. “What’s different this time is we are seeing much younger people in the hospital,” Ennis said. Vaccination rates have typically been higher in older age groups. Across Alabama, the number of COVID-19 patients in state hospitals jumped from 213 on July 4 to 1,802 on Aug. 4, according to the Alabama Hospital Association. The current hospitalization numbers are far less than the 3,000 COVID-19 patients in state hospitals at the peak of the pandemic in January. However, health officials have expressed concern about the steep upward trend. As of Wednesday, there were 508 patients in state hospitals, compared to 848 on Jan. 12, said Dr. Don Williamson, head of the Alabama Hospital Association. Alabama ranked fifth in the nation for new cases per capita in the past 14 days, according to researchers at Johns Hopkins University. The seven-day rolling average of daily new cases in Alabama has risen over the past two weeks from 1,013.71 new cases per day on July 19 to 2,525.71 new cases per day on Aug. 2. People who have been vaccinated can contract the coronavirus, but health officials have said they are far less likely to get seriously ill. Dr. Jeremy Rogers, an emergency room physician and director of clinical services at Grandview Medical Center, said 92% of incoming COVID patients at his facility are unvaccinated, and a majority are under age 60. He said they recently admitted a 19-year-old with COVID. “This is absolutely heartbreaking what we are seeing. It’s tragic. And unfortunately, it’s largely preventable,” Rogers said. “We’ve talked a lot about vaccine hesitancy, but I’ve seen a lot of vaccine regret in patients, in family members that wish they would have been vaccinated sooner. Vaccines are widely available, and so now’s the time to get vaccinated before it’s too late,” Rogers said. Dr. Timothy Bode, chief medical officer at Ascension St. Vincent’s Health System, said 88% of their nearly 100 COVID-19 patients are unvaccinated. He said 93% of COVID-19 patients in critical care units and on ventilators are unvaccinated. Dr. Mark Wilson, health officer for the Jefferson County Department of Health, urged people to get vaccinated and to get back to basics with wearing masks and avoiding crowds. “We are in a big scary surge right now,” Wilson said. Republished with the permission of the Associated Press.
Virus hospitalizations in Alabama approach 1,600 amid surge
The number of coronavirus patients in Alabama hospitals rose to its highest levels in six months Monday as health officials urged schools to require masks and other measures during a “critical juncture” in the pandemic. Dr. Don Williamson, the former state health officer who now heads the Alabama Hospital Association, said the 1,583 hospitalized people include 38 children. The state last saw numbers that high in early February. A month ago, there were a little over 200 people hospitalized. The 1,583 patients in state hospitals is a little more than half of the number in January when there were 3,000 hospitalized. But Williamson said he is concerned the state is rapidly approaching the previous high-water mark. Alabama’s status as one of the two least vaccinated states in the country — plus studies suggesting that the delta variant is just a contagious as chickenpox and that even vaccinated people can spread the illness to others — have caused health officials to worry about what is ahead and to emphasize the need for mask-wearing and vaccinations. Alabama, in the last two weeks, has seen one of the sharpest rises in COVID-19 cases in the country, ranking eighth among the states, according to researchers at Johns Hopkins University. The seven-day rolling average of daily new cases in Alabama has risen over the past two weeks from 799.57 new cases per day on July 17 to 2,391.14 new cases per day on July 31. Only 34.4% of Alabama’s population is fully vaccinated, which is the lowest percentage in the nation, according to numbers from the U.S. Centers for Disease Control and Prevention. Mississippi has 34.5% of its population fully vaccinated. The Alabama Department of Public Health Monday officially released guidance that encourages K-12 public schools to implement universal masking, including on school buses, when classes resume. Dr. Karen Landers, a medical officer and pediatrician with the Alabama Department of Public Health, wrote that it is imperative for adults to take action since children under age 12 are not eligible for the vaccine. “With low vaccine rates in Alabama, it will be a matter of a few weeks after school resumes before we see a rise in cases in the educational system,” Landers wrote in the document. “Alabama is at a critical juncture. All of us want our children to be able to learn and thrive,” she wrote. Gov. Kay Ivey Monday also released a video with State Health Officer Scott Harris answering questions about the vaccine and encouraging people to get vaccinated. “Because we have this delta variant circulating, it is so infectious that anybody who gets it is likely to spread it to three or four other people,” Harris said. Republished with the permission of the Associated Press.

