U.S. health experts urge flu shots to avoid ‘twindemic’
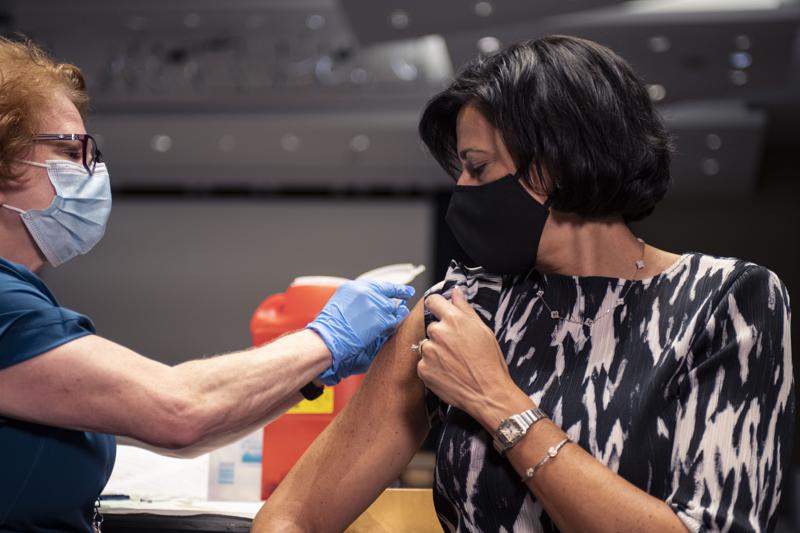
The U.S. is gearing up for a possible bad flu season on top of the continuing COVID-19 crisis, with a plea Thursday for Americans to get vaccinated against both. “I get it: We are all tired of talking about vaccines,” said Dr. Rochelle Walensky, director of the Centers for Disease Control and Prevention. But “it is doubly important this year” to get your flu shot, added Walensky, who got her own vaccination earlier this week just as she has every year since she was a medical student in 1995. “We are preparing for the return of the flu.” Flu cases dropped to historically low levels globally over the pandemic, as restrictions designed to slow the spread of the coronavirus helped block other respiratory viruses. But with schools and businesses reopened, international travel resuming, and far less masking, there’s no way to predict how bad a flu season the U.S. might expect this winter. But officials are worried because a different respiratory virus named RSV, which usually attacks young children in the winter, instead roared back last summer as soon as people started dropping their masks. “Is that a harbinger of a worse influenza season? We don’t know, but we certainly don’t want a ‘twindemic,’ both COVID and influenza,” said Dr. William Schaffner of the National Foundation for Infectious Diseases. And if you still need a COVID-19 vaccination — either first shots or a booster dose — you can get it at the same visit as a flu shot. The CDC recommends a yearly flu vaccination for just about everyone starting with 6-month-old babies. Influenza is especially dangerous for older adults, children under age 5, people with chronic health problems such as diabetes, asthma, or heart disease, and during pregnancy. Last fall, about as many Americans overall got their flu vaccination as they did before the pandemic — about half of the eligible population, according to CDC data released Thursday. But Walensky was dismayed by a slight drop in child flu vaccinations last year — and at widening racial and ethnic disparities. Last year, 43% of Black Americans and 45% of Hispanics got a flu vaccination compared to 56% of whites. The CDC expects vaccine makers to deliver 188 million to 200 million doses of flu vaccine. Most Americans with insurance can get one without a co-pay. Options include regular shots, shots that aim to give older adults a little extra protection, and a nasal spray. All offer protection against four different flu strains that global experts predict are the kinds most likely to spread this year. At the same time they get vaccinated against flu, officials also urged older adults and people with chronic illnesses to ask about getting a vaccine against a type of pneumonia that is a frequent complication. Republished with the permission of the Associated Press.
U.S. health officials call for booster shots against COVID-19
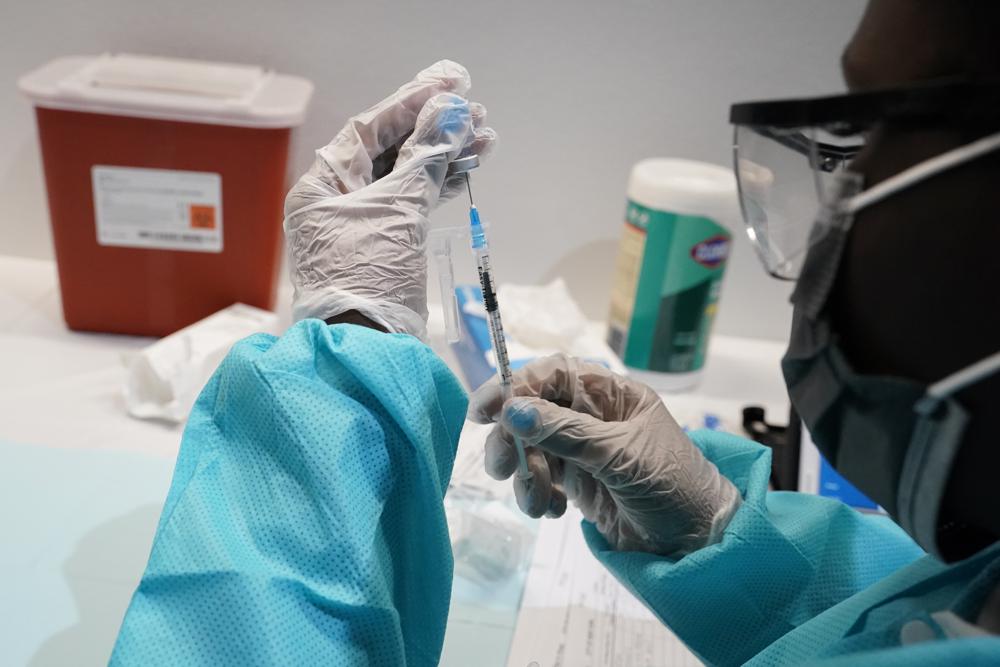
U.S. health officials Wednesday announced plans to dispense COVID-19 booster shots to all Americans to shore up their protection amid the surging delta variant and signs that the vaccines’ effectiveness is slipping. The plan, as outlined by the chief of the Centers for Disease Control and Prevention and other top health authorities, calls for an extra dose eight months after people get their second shot of the Pfizer or Moderna vaccine. The doses could begin the week of Sept. 20. “Our plan is to protect the American people, to stay ahead of this virus,” CDC Director Dr. Rochelle Walensky said as the agency cited a raft of studies suggesting that the vaccines are losing ground while the highly contagious variant spreads. People who received the single-dose Johnson & Johnson vaccine will also probably need extra shots, health officials said. But they said they are waiting for more data. Officials said that before any booster program starts up, the Food and Drug Administration and a CDC advisory panel would need to evaluate the safety and effectiveness of an extra dose. “We have a responsibility to give the maximum amount of protection,” President Joe Biden said at the White House. He added that extra doses are also “the best way to protect ourselves from new variants that could arise.” The announcement came the same day the Biden administration said it would require nursing homes to mandate vaccinations for staffers in order to continue receiving federal funds. Hundreds of thousands of nursing home workers remain unvaccinated, despite the heightened risk of fatal infections among elderly residents. Officials said it is “very clear” that the vaccines’ protection against infections wanes over time, and they noted the worsening picture in Israel, which has seen a rise in severe cases, many of them in people already inoculated. They said the U.S. needs to get out ahead of the problem before it takes a more lethal turn here and starts leading to increasing hospitalizations and deaths among the vaccinated. Dr. Anthony Fauci, the government’s foremost expert on COVID-19, said one of the key lessons of the coronavirus is that it’s better to “stay ahead of it than chasing after it.” The first boosters would go to people in high-priority groups that received the initial U.S. vaccinations: nursing home residents, health workers, and those with underlying health conditions. Health officials are likely to recommend that the booster be the same brand of vaccine that people received initially. Dr. Mark Mulligan of NYU’s Langone Health center welcomed the announcement, saying: “Part of leadership is being able to see around the corner and make hard decisions without having all the data. It seems to me that’s what they’re doing here.” Top scientists at the World Health Organization bitterly objected to the U.S. plan, noting that poor countries are not getting enough vaccine for their initial rounds of shots. “We’re planning to hand out extra life jackets to people who already have life jackets, while we’re leaving other people to drown without a single life jacket,” said Dr. Michael Ryan, the WHO’s emergencies chief. The organization’s top scientist, Dr. Soumya Swaminathan, said the evidence does not show boosters are needed for everyone, and she warned that leaving billions of people in the developing world unvaccinated could foster the emergence of new variants and result in “even more dire situations.” U.S. Surgeon General Vivek Murthy rejected the notion that the U.S. must choose between “America and the world,” saying: “We clearly see our responsibility to both.” White House officials noted that the U.S. has donated 115 million doses to 80 countries, more than all other nations combined. They said the U.S. has plenty of vaccine to dispense boosters to its own population. Israel is already offering booster shots to people over 50. And European regulators are looking into the idea. Last week, U.S. health officials recommended a third shot for some people with weakened immune systems, such as cancer patients and organ transplant recipients. Offering boosters to all Americans would be a major expansion of what is already the biggest vaccination campaign in U.S. history. Nearly 200 million Americans have received at least one shot. Some experts have expressed concern that calling for boosters would undermine the public health message — and reinforce opposition to the vaccine — by raising more doubts in the minds of people already skeptical about the shots’ effectiveness. As for why the vaccines appear to be less effective over time at stopping infections, there are indications that the body’s immune response to the shots fades, as it does with other inoculations. But also, the vaccines simply may not protect against the delta variant as well as they do against the original virus. Scientists are still trying to answer the question. Officials said the eight-month timeframe was a judgment call about when vaccine protection against severe illness might fall, based on the direction of the current data. “There’s nothing magical about this number,” the surgeon general said. Nearly 20 months into the outbreak, the scourge has killed 620,000 Americans. Just weeks after the president declared the country’s “independence” from COVID-19 on July Fourth, emergency rooms in parts of the South and West are overloaded again, and cases are averaging nearly 140,000 per day, quadrupling in just a month. In making its announcement, the CDC released a number of studies conducted during the delta surge that suggest that the vaccines remain highly effective at keeping Americans out of the hospital but that their ability to prevent infection is dropping markedly. One of the studies looked at reported COVID-19 infections in residents of nearly 15,000 nursing homes and other long-term care facilities. It found that the effectiveness of the Pfizer and Moderna vaccines against infection fell from about 74% in March, April, and early May to 53% in June and July. The study examined all COVID-19 infections, with or without symptoms. The researchers said more work is needed to determine if there was a higher incidence of infections that resulted in
Vaccinations rise in some states with soaring infections

Vaccinations are beginning to rise in some states where COVID-19 cases are soaring, White House officials said Thursday in a sign that the summer surge is getting the attention of vaccine-hesitant Americans as hospitals in the South are being overrun with patients. Coronavirus coordinator Jeff Zients told reporters that several states with the highest proportions of new infections have seen residents get vaccinated at higher rates than the nation as a whole. Officials cited Arkansas, Florida, Louisiana, Missouri, and Nevada as examples. “The fourth surge is real, and the numbers are quite frightening at the moment,” Louisiana Gov. John Bel Edwards said on a New Orleans radio show. Edwards, a Democrat, added: “There’s no doubt that we are going in the wrong direction, and we’re going there in a hurry.” Louisiana reported 2,843 new COVID-19 cases Thursday, a day after reporting 5,388 — the third-highest level since the pandemic began. Hospitalizations are up steeply in the last month, from 242 on June 19 to 913 in the latest report. Fifteen new deaths were reported Thursday. Just 36% of Louisiana’s population is fully vaccinated, state health department data shows. Nationally, 56.3% of Americans have received at least one dose of the vaccine, according to the Centers for Disease Control and Prevention. Aly Neel, a spokesperson for Louisiana’s health department, said the state has seen “a little bump” in vaccinations recently, adding that details would be available Friday. Warner Thomas, president and CEO of the Ochsner Health system serving Louisiana and Mississippi, said the system had seen a 10% to 15% increase in people seeking vaccination over the past week or two. It has administered vaccines at churches, the New Orleans airport, basketball games, and the mall. “We see each person we get vaccinated now as a victory,” said Dr. Katherine Baumgarten, director of infection prevention and control for the 40-hospital system, noting that it has been bringing in traveling nurses and that projections show its ICUs could fill up at the current rate of infection. Dr. Catherine O’Neal, chief medical officer and an infectious disease specialist at Our Lady of the Lake regional medical center, said Thursday that the most shocking aspect of the surge has been its speed. The caseload has roughly tripled in the course of a week, she said. On Sunday, the medical center stopped taking transfers of coronavirus patients from hospitals in other parts of the state because they simply did not have the capacity, she said. In Missouri, which is second only to Arkansas and Louisiana in the number of new cases per capita over the past 14 days, officials have rolled out a vaccine incentive program that includes $10,000 prizes for 900 lottery winners. The state lags about 10 percentage points behind the national average for people who have received at least one shot. Hospitals in the Springfield area are under strain, reaching pandemic high and near pandemic high numbers of patients. “Younger, relatively healthy, and unvaccinated. If this describes you, please consider vaccination,” tweeted Erik Frederick, chief administrative officer of Mercy Hospital Springfield, noting that half of the COVID-19 patients are ages 21 to 59, and just 2% of that group is vaccinated. The surge that began in the southwest part of the state, where some counties have vaccination rates in the teens, has started to spread to the Kansas City area, including at Research Medical Center. “I don’t want to keep putting my life on the line just because people don’t want to get vaccinated or listen to what health care professionals are recommending,” lamented Pascaline Muhindura, a registered nurse who has worked on the hospital’s COVID-19 unit for more than a year. “A lot of them don’t even believe in COVID-19 to begin with. It is incredibly frustrating. You are helping someone that doesn’t even believe that the illness that they have is real,” Muhindura said. Dr. Jason Wilson, an emergency physician with Tampa General Hospital, also has watched the rise in cases with frustration. Unlike earlier in the pandemic, when many patients were in their 70s, he has seen the median patient age fall to the mid-40s. “I spent a lot of time this fall and last summer saying, ’We’ve got to do these things, these social mitigation strategies until we get that vaccine. Just hang in there,” Wilson said. Hospitals initially were hopeful as cases declined. But then, he said, “Things just fell flat.” Conservative Utah reported Wednesday that almost 300 people were hospitalized due to the virus — the highest number in five months. Intensive care units reached 81.5% capacity. Health officials renewed their pleas for residents to get vaccinated. One of Arizona’s biggest hospital systems issued its own call for vaccinations, citing an increase in seriously ill COVID-19 patients in just a few weeks. Dr. Michael White of Valleywise Health said doctors were mostly treating people with moderate symptoms, but that began to change two weeks ago. Now patients arrive acutely ill. “This delta at the moment it is honing in on largely unvaccinated persons,” said Dr. William Schaffner, a professor of infectious diseases in the health policy department at the Vanderbilt University School of Medicine in Nashville. The variant, which originated in India, now accounts for an estimated 83% of coronavirus samples genetically identified in the U.S. It is the predominant strain in every region of the country and continues “spreading with incredible efficiency,” the director of the CDC, Dr. Rochelle Walensky, told reporters at the White House. She said the mutation is more aggressive and much more transmissible, calling it “one of the most infectious respiratory viruses we know of.” “We are yet at another pivotal moment in this pandemic,” she warned. “We need to come together as one nation.” The CDC has not changed its guidance that vaccinated people do not need to wear masks. But in Georgia, Atlanta Public Schools announced Thursday that it will implement a “universal mask-wearing” policy in all of the system’s school buildings when fall classes begin. Just 18%

